Hip PainAdelaide
Hip pain is rarely just a hip problem. The lower back, the pelvis, and the gluteal tendons often share the load with the hip joint itself. Research suggests assessment should consider the full kinetic chain, not the hip in isolation. $69 initial consultation with Dr Sam Johnson (Chiropractor). No referral needed.

Does this sound familiar?
Common hip pain patterns we hear. Tap a card for a plain-English explanation.
"Groin and front-of-hip stiffness that is worst first thing in the morning, then eases a bit as I move."
"Lateral hip pain over the bony point. I cannot lie on that side at night."
"Sharp groin pinch when I squat, sit in a low chair, or drive for more than 30 minutes."
"Deep buttock or posterior hip ache that feels connected to my lower back."
What Hip Pain Looks Like
Hip pain covers a regional cluster of mechanical patterns. The hip joint, the gluteal tendons, the lumbar spine, and the sacroiliac region all refer pain into the same area. The job of assessment is to sort out which pattern fits.
Typical features we hear about include:
- Location ranging from the groin, the front of the hip, the bony point on the side of the hip (greater trochanter), the buttock, or referral into the thigh or knee.
- Aggravators including prolonged sitting, stairs, deep hip flexion (squatting, getting in and out of a low chair), lying on the affected side at night, walking on uneven ground, and getting out of the car.
- Easing often with gentle movement, warm showers, short walks, and avoiding the direct provocation for a few days.
- Morning stiffness is common with hip osteoarthritis and tends to ease with gentle movement over 15 to 30 minutes.
- Night pain on the affected side is a common feature of lateral hip pain (greater trochanteric pain syndrome) and waking because of the hip is a common trigger for seeking care.
Sorting Out Which Pattern Fits
Hip pain is an umbrella. The more specific patterns below each behave differently and respond to different emphasis in care. Naming the pattern helps shape the plan.
| Pattern | Typical Location | Typical Aggravators | What Research Suggests |
|---|---|---|---|
| Hip osteoarthritis | Groin, front of hip, sometimes thigh and knee | Stairs, prolonged sitting, twisting, morning stiffness | Manual therapy plus exercise may help manage pain and function |
| Greater trochanteric pain syndrome (gluteal tendinopathy) | Bony point on the side of the hip, radiating down outer thigh | Side-lying at night, crossing legs, walking on a slope | Progressive gluteal loading is first-line and may outperform cortisone injection |
| Femoroacetabular impingement (FAI) | Groin, occasional C-sign grip around the hip | Deep squat, low chair, long car trips, kicking a ball | Physiotherapy-style rehab may help many; orthopaedic opinion if plateau |
| Referred from lumbar or sacroiliac | Buttock, posterior hip, sometimes into thigh | Bending, twisting, sustained positions, sneezing | Assessment looks at hip, lumbar, and SI together as a kinetic chain |
Assessment may find one pattern dominant, or a mix of contributors. Care is tailored to what the examination finds, not to the label alone.
How We Assess Hip Pain
A structured bedside examination looks at the hip, lumbar spine, and sacroiliac region together. The goal is to identify the dominant contributor and rule out anything that warrants urgent medical review.
A typical assessment includes:
- History screen covering onset, pattern of pain, aggravators, night pain, work and activity load, prior hip or back history, and any red-flag features.
- Hip range and strength testing in flexion, extension, abduction, and rotation, including gluteal strength and provocation tests for FAI and gluteal tendinopathy.
- Lumbar and sacroiliac screen with range, palpation, and movement patterns, as research suggests the lumbar spine and SI joint are common sources of referred hip pain.
- Gait and functional observation watching sit-to-stand, single-leg stance, and a short walk, looking for Trendelenburg pattern and compensatory movement.
- Red-flag screen for infective, inflammatory, neoplastic, fracture, vascular, and neurological presentations that sit outside musculoskeletal scope.
After the examination, findings are explained in plain English, along with what we think is driving the pattern and what the options are. If imaging, a GP review, an orthopaedic opinion, or a rheumatology review would add useful information, we will say so.
What the Research Suggests
Conservative manual therapy, graded exercise, and load guidance feature in mainstream guidelines for musculoskeletal hip pain. The studies below summarise what the research suggests, not what any individual person will experience.
Courtney 2022 · JOSPT
Manual therapy plus exercise may offer small added benefit for hip and knee OA
Systematic review with meta-analysis of RCTs suggesting manual therapy added to exercise may produce small additional short-term benefits on pain and function for hip and knee osteoarthritis compared with exercise alone. Individual responses vary.
Read the study →Mellor 2018 · BMJ
Exercise may outperform cortisone for greater trochanteric pain syndrome
LEAP randomised controlled trial of 204 adults with lateral hip pain. Progressive exercise and education produced higher global improvement at 8 weeks and greater sustained improvement at 52 weeks compared with cortisone injection or wait-and-see.
Read the study →Griffin 2018 · Lancet (FASHIoN)
Hip arthroscopy and personalised physio both produced improvement for FAI
Multicentre RCT of 348 adults with femoroacetabular impingement. Both hip arthroscopy and personalised physiotherapy produced improvement; arthroscopy showed statistically greater improvement at 12 months. Both are legitimate first-line choices in many presentations.
Read the study →Bennell 2014 · JAMA
Multimodal physical therapy may help manage hip OA pain
Randomised controlled trial of adults with hip osteoarthritis. Multimodal physical therapy (manual therapy, education, and home exercise) produced improvement in pain and function compared with sham, though effect sizes were modest. Individual responses vary.
Read the study →Mallows 2024 · Physiotherapy
Exercise may slightly reduce pain and improve function in GTPS
Systematic review and meta-analysis of RCTs for greater trochanteric pain syndrome. Exercise produced a small improvement in pain and function versus control, shockwave, or injection comparators. Progressive tensile loading is the current evidence-backed approach.
Read the study →Abbott 2013 · Osteoarthritis Cartilage (MOA)
Manual therapy plus exercise may help hip OA short-term
MOA randomised controlled trial of 206 adults with hip or knee OA. Manual therapy combined with exercise therapy produced clinically meaningful short-term improvements in pain and function. Effects tapered at 12 months, so ongoing self-management matters.
Read the study →Mintken 2017 · J Orthop Sports Phys Ther
Thrust and non-thrust manipulation for hip OA
Clinical practice guideline noting manual therapy (including mobilisation and, where appropriate, manipulation) combined with exercise may be useful for patients with mild to moderate hip osteoarthritis. Individual clinical reasoning guides technique selection.
Read the guideline →Bialosky 2018 · JOSPT
How manual therapy may produce its effects
Updated model proposing manual therapy effects involve neurophysiological mechanisms (peripheral, spinal, supraspinal) alongside mechanical change. Supports using manual therapy as one part of a wider active-rehab plan rather than a standalone intervention.
Read the model →How Chiropractic Care May Help
Research suggests conservative manual therapy, combined with graded loading and load guidance, may help manage musculoskeletal hip pain. Care is tailored to how your hip, lumbar spine, and sacroiliac region respond to assessment. Individual responses vary.
At Stapleton Chiropractic, care for hip pain typically includes:
- Detailed history and red-flag screen to confirm the presentation is mechanical and to rule out anything that warrants urgent medical review.
- Hip and pelvis mobilisation using gentle techniques, with attention to the lumbar spine and sacroiliac region as common kinetic-chain contributors.
- Low-force options using an Activator instrument or drop-piece table where appropriate. Both are well-tolerated and suited to an irritated or guarded hip.
- Diversified manual adjustment for patients comfortable with hands-on adjusting, applied to the lumbar spine, sacroiliac region, and thoracolumbar junction as clinically indicated.
- Soft tissue techniques for the gluteal muscle bellies, tensor fascia lata, iliotibial band, and lumbar paraspinal regions that often guard around an irritated hip.
- Graded loading and lifestyle guidance for work, sleep positions, and activity, so the aggravators settle while the tissues recover. For lateral hip pain, this includes advice on side-lying sleep posture and avoidance of leg-crossing during a flare.
Progress is reviewed at each visit. There are no lock-in plans, and the decision to continue is always yours. If your response to care is not what we would expect, we will reassess and, where appropriate, discuss referral pathways back to your GP, to imaging, to an orthopaedic opinion, or to a colleague in another discipline.
Chiropractic vs Physiotherapy vs GP plus Orthopaedic Surgeon
Hip pain care is almost always a team sport. Here is where each role typically sits.
| What you get | Chiropractic (Stapleton) | Physiotherapy | GP plus Orthopaedic Surgeon |
|---|---|---|---|
| Primary focus | Mechanical hip pain, kinetic-chain assessment, low-force manual therapy plus exercise guidance | Exercise-first rehab, progressive loading, movement retraining | Diagnosis, imaging, medical and surgical management (e.g. hip replacement, arthroscopy) |
| Manual therapy | Low-force options (Activator, drop-piece), gentle mobilisation, soft tissue work | Soft tissue work, gentle mobilisation; some physios use manipulation | Not the typical role; focus is on medical and surgical care |
| Exercise prescription | Yes, short home-based routines tailored to the hip and the broader kinetic chain | Yes, often higher volume, progressive loading, and rehab programming | Typically referred out to allied health |
| Lock-in plans | No. Visit by visit; the decision is always yours | Varies by clinic | Not applicable |
| Imaging and medication | We coordinate; we do not prescribe or order | Usually coordinate; do not prescribe | Full scope, including joint injection and referral to imaging |
| Surgical pathway | We refer when indicated, including for severe OA or mechanical locking | Refer through GP; rehab pre and post surgery | Primary surgical decision-makers for hip replacement and arthroscopy |
| Health fund rebates | Yes, all major funds | Yes, all major funds | Medicare plus private; some procedures claimable |
If we feel you would benefit from a different approach, we will always let you know. Cold laser (ACL11 Cold Laser) operates from the same building and may be discussed during consultation when suitable for tendon-related hip pain.
Why Stapleton Chiropractic
Adult-first, evidence-informed, and family-run since 1972. No lock-in plans, clear pricing, and the decision is always yours.
Est. 1972
Over five decades on Marion Road. A Plympton Park practice your family likely already knows.
Evidence-informed
Care is guided by clinical practice guidelines and musculoskeletal research. Outcomes are discussed honestly.
No lock-in plans
Pay per visit. The decision to continue is always yours, reviewed at each appointment.
Transparent pricing
$69 initial consultation, $60 standard. All major health funds accepted with on-the-spot claiming where supported.
What Your First Visit Looks Like
Four straightforward steps. No paperwork marathons, no surprises.
Book online or call
Pick a time that suits. No referral needed. $69 initial consultation.
Brief intake
Short history form at reception, covering the pain story and any red flags.
Assessment
Examination of hip, lumbar spine, and sacroiliac region. We explain what we find.
Discussion & next steps
Plain-English findings and options. If care is appropriate, we discuss it. The decision is always yours.
Ready to speak to Dr Sam?
$69 initial consultation. No lock-in plans. All major health funds accepted.
Book a ConsultationTransparent Affordable Fees
No lock-in plans, no pressure. Fees sit well below the South Australian average.
Source: Australian Chiropractors Association Consultation Fee Survey 2025 (SA data). All major health funds accepted.
Warning Signs That Warrant Urgent Medical Review
Most hip pain is mechanical and not an emergency. A small number of presentations do need urgent medical review, because hip pain may occasionally be the presenting feature of something more serious.
Seek urgent medical review (GP, healthdirect 1800 022 222, or emergency department) if your hip pain is accompanied by any of the following:
- Fever, night sweats, or malaise alongside a hot, swollen, very tender hip. May suggest septic arthritis, which is a medical emergency.
- Inability to bear weight after a fall, trauma, or twist. May suggest fracture and warrants imaging before any manual therapy.
- Severe night pain unrelieved by rest, pain that wakes you regularly and does not settle with position change. May warrant GP review for investigation.
- Unexplained weight loss, history of cancer, or new bony hip pain that feels different from prior musculoskeletal pain. May warrant prompt imaging.
- Progressive weakness, numbness, or loss of bladder or bowel control. May suggest a serious neurological cause including cauda equina syndrome; emergency department review is appropriate.
- Sudden groin and front-of-thigh pain with pale, cold, or pulseless lower limb. May suggest vascular compromise; emergency department review is appropriate.
- Known immunosuppression, recent joint injection, or intravenous drug use with new hip pain. May raise the suspicion of joint infection.
- Children with hip pain, fever, and a limp. Always warrants urgent GP or emergency review.
If any of these apply, please do not wait for a chiropractic appointment. Contact your GP, call healthdirect on 1800 022 222, or attend your nearest emergency department. These features may indicate a condition that warrants urgent medical review, rather than a mechanical hip issue. When in doubt, please speak to your GP first.
Ready to Get Started? We're Ready When You Are.
Choose a time that works for you. No referral needed.

Dr Sam Johnson (Chiropractor)
B.Sc.(Chiro), M.Chiro.(Macq)
$69
Initial Consultation
Up to 30 minutes, including full assessment
Book Your First VisitPrefer to call? (08) 8297 5277
Text: 0400 105 454 | Email: wecanhelp@stapletonchiropractic.com.au
You will receive a confirmation email with all details immediately after booking.
Frequently Asked Questions
Is my hip pain coming from my lower back?
Do I need imaging for hip pain?
When should I see a GP instead of a chiropractor for hip pain?
Can a chiropractor help with hip osteoarthritis?
What is greater trochanteric pain syndrome and can it be helped?
What is FAI and what should I do about it?
Should I keep exercising if my hip hurts?
What happens at a first consultation?
How much does a chiropractic consultation cost?
Do I need a GP referral?
Ready to Take the First Step?
Book your initial consultation with Dr Sam Johnson (Chiropractor). No referral needed. $69 initial consultation.
Stapleton Chiropractic. Est. 1972. Clinically led by Dr Sam Johnson (Chiropractor), BSc (Chiropractic) and MChiro, Macquarie University. AHPRA-registered.
Address: 528 Marion Road, Plympton Park SA 5038 Phone: (08) 8297 5277 Hours: Mon to Fri 7am to 7pm, Sat 8am to 12pm Email: wecanhelp@stapletonchiropractic.com.au
Scope note: We focus on the assessment and conservative management of musculoskeletal conditions. We do not make claims about non-musculoskeletal conditions.
What to Expect at Your First Visit
Stapleton Chiropractic is an evidence-based chiropractic practice at 528 Marion Road, Plympton Park, Adelaide (Est. 1972). An initial consultation costs $69 and includes a comprehensive 30-minute hands-on assessment. All major health funds accepted; no referral needed.
Allow up to 30 minutes for a comprehensive initial consultation. Here is how it works.
You Tell Us
We listen carefully, ask the right questions, and build a clear picture of what has been going on.

We Assess
Hands-on testing and biostructural analysis to identify what may be contributing to your concern.
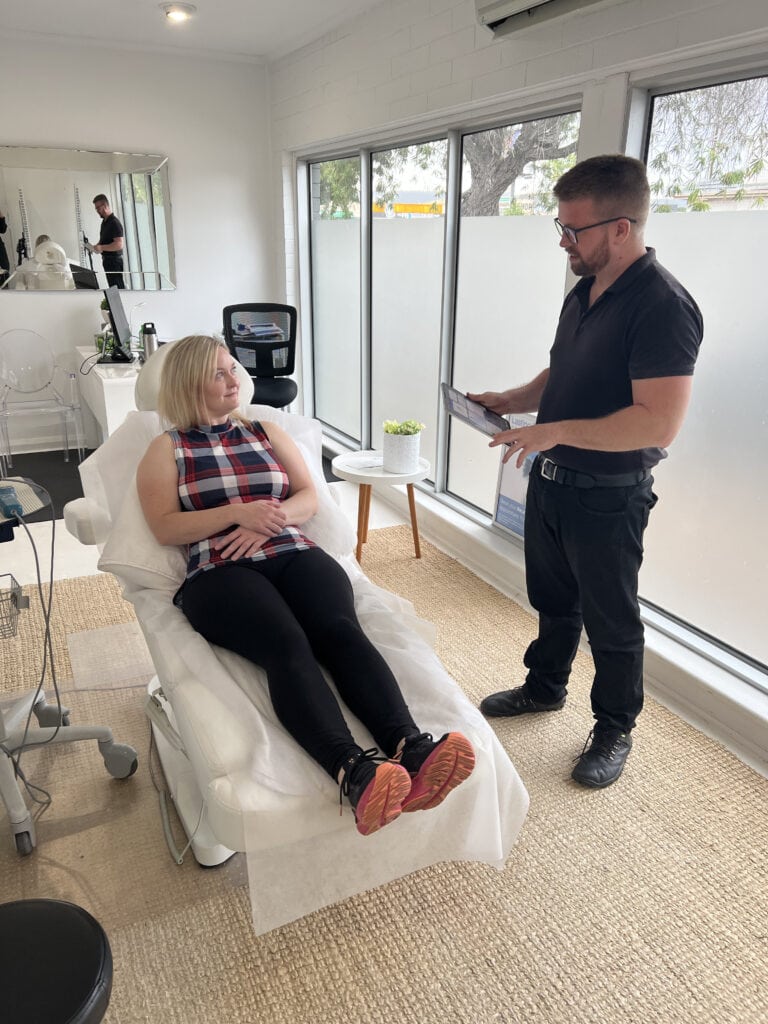
We Explain
We walk you through our findings and your options in plain language. If imaging is recommended, we will explain why and discuss your options.
X-rays are only referred for with your consent, and where eligible, may be bulk billed.*

Care May Begin
Where clinically appropriate, care may begin on your first visit to help support relief.*
We offer both traditional hands-on chiropractic techniques and gentle, low-force approaches, tailored to your comfort. Care only proceeds with your consent.
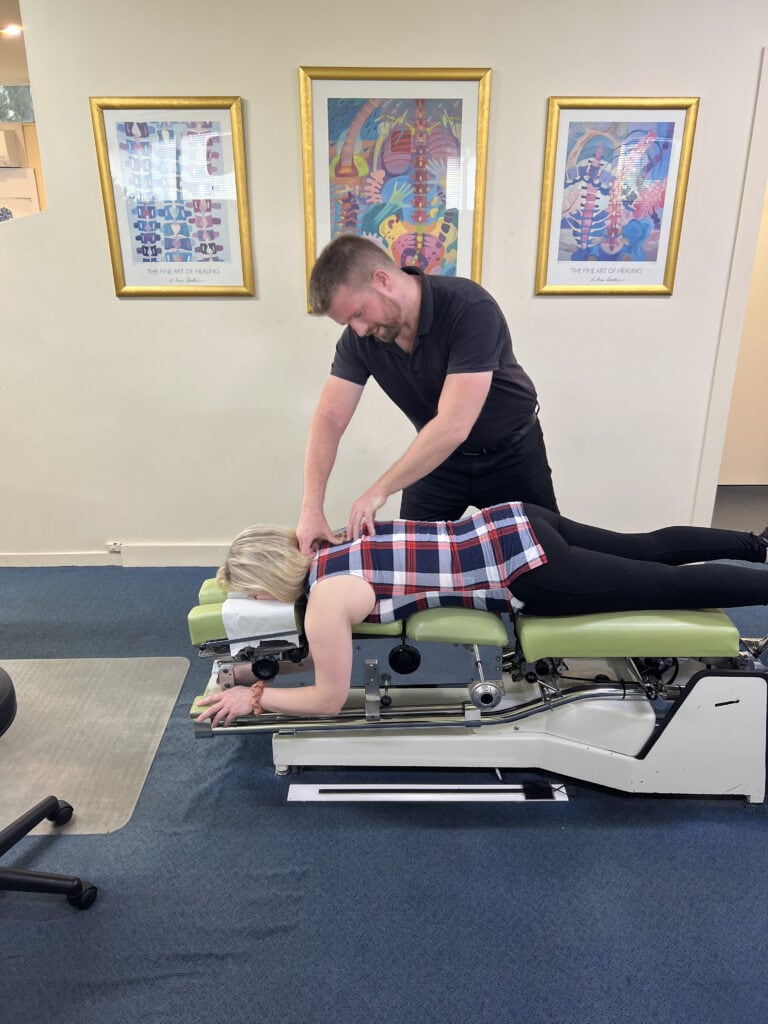
Ready to Get Started?
Your first visit takes about 30 minutes. No referral needed, no lock-in plans. The decision is always yours.
Book Your First Visit*Subject to clinical assessment and suitability criteria. Bulk billing subject to eligibility criteria and clinical need.
Transparent Affordable Fees
Source: Australian Chiropractors Association Consultation Fee Survey 2025 (SA data). *Care provided where clinically appropriate, subject to assessment.
Care that fits your day
528 Marion Road, Plympton Park SA 5038
Ready to Get Started? We're Ready When You Are.
Choose a time that works for you. No referral needed.

Dr Sam Johnson (Chiropractor)
B.Sc.(Chiro), M.Chiro.(Macq)
$69
Initial Consultation
Up to 30 minutes, including full assessment
Book Your First VisitPrefer to call? (08) 8297 5277
Text: 0400 105 454 | Email: wecanhelp@stapletonchiropractic.com.au
You will receive a confirmation email with all details immediately after booking.
