Cervicogenic Headache Chiropractor in Adelaide


If your headaches always seem to start in the base of your skull or upper neck, worsen when you turn or hold your head in one position, and sit on one side of your head, you are describing a pattern that research suggests may indicate a cervicogenic headache. I have spent over 10 years at Stapleton Chiropractic assessing patients whose headaches were never properly linked back to the neck. Many had tried medication, massage, or optometry appointments first. A careful upper-cervical assessment is often the missing step.
My priority when you walk in is simple: help you feel better. From there, I take the time to explain what I am finding, what may be contributing, and what your options look like. Then the decision is yours. I will map out the path, but you are always in control.
I completed my Bachelor of Chiropractic Science and Master of Chiropractic at Macquarie University in Sydney. I work with people across all ages and walks of life, and I am as happy to co-manage your care with your GP as I am to refer on if something else suits you better.
If you have any questions, feel free to get in touch with our friendly team. I look forward to helping you work out whether your cervicogenic headaches may be neck-related.
Dr Sam Johnson (Chiropractor)
Principal Chiropractor, Stapleton Chiropractic
That one-sided headache that flares when you turn your head? It may be starting in your upper neck, not your head. Cervicogenic headaches refer pain from the upper cervical spine (C1 to C3) into the head via shared nerve pathways. At Stapleton Chiropractic, we take a detailed history, perform a hands-on assessment of your upper neck, and explain what we find in plain language before discussing your options.
Yes, chiropractors in Adelaide commonly assess and manage cervicogenic headache, a headache pattern that research suggests may arise from dysfunction in the upper cervical spine (C1 to C3). The 2026 clinical practice guideline published in the Journal of Integrative and Complementary Medicine recommends spinal manipulation as a primary intervention for this specific headache type.[1]
Cervicogenic headache typically presents on one side of the head, is provoked or worsened by neck movement, and is often accompanied by restricted neck range of motion. Your initial assessment at Stapleton Chiropractic includes a detailed headache history, red flag screening, and a hands-on examination of your upper cervical spine. The goal is to build a clear picture of whether mechanical factors may be contributing so we can discuss your options in plain language.
Why a problem in your upper neck can feel like a headache
The nerves from the top three vertebrae in your neck (C1, C2 and C3) share a relay station in the brainstem with the trigeminal nerve, which supplies sensation to your face, forehead and the top of your head. This shared relay is known as the trigeminocervical nucleus. When the nerves of your upper neck are irritated, the brain can interpret the signal as pain coming from the head rather than the neck. Clinicians refer to this as referred pain.
Research suggests cervicogenic headache may account for 15 to 20% of chronic headaches and is frequently underdiagnosed because the pain is felt in the head, not where the underlying dysfunction sits. Common mechanical contributors include sustained forward-head posture, prior neck trauma, restricted upper cervical joints, and tension in the suboccipital muscles at the base of the skull. Individual presentations vary.
*General information only. This is not a diagnosis and does not replace a proper clinical assessment. Individual presentations vary.
Does this sound familiar?
What to Expect at Your First Visit
Your first visit is a 30-minute consultation costing $69. It includes a detailed headache history, a hands-on assessment of your upper cervical spine, suboccipital muscles, and upper thoracic region, a plain-language explanation of findings, and treatment on the same day where clinically appropriate. No referral is needed, and the decision about care is always yours.
Allow up to 30 minutes for a comprehensive initial consultation. Here is how it works.
You Tell Us
We listen carefully, ask the right questions, and build a clear picture of what has been going on with your neck.

We Assess
Hands-on testing and biostructural analysis to help work out whether mechanical factors in your neck may be contributing to your headaches.
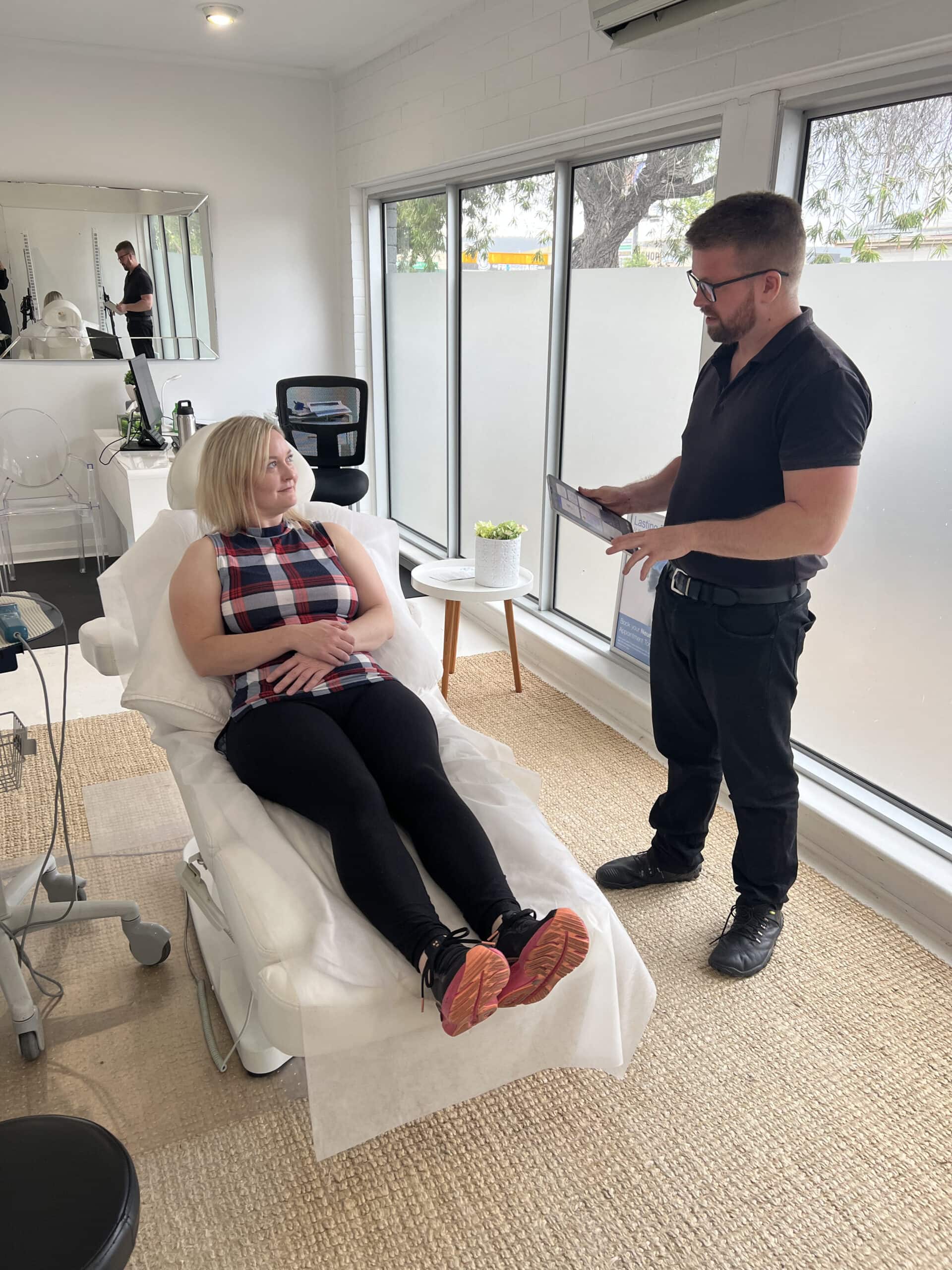
We Explain
We walk you through our findings and your options in plain language. If imaging is recommended, we will explain why and discuss your options.
X-rays are only taken with your agreement, and where eligible, may be bulk billed.*

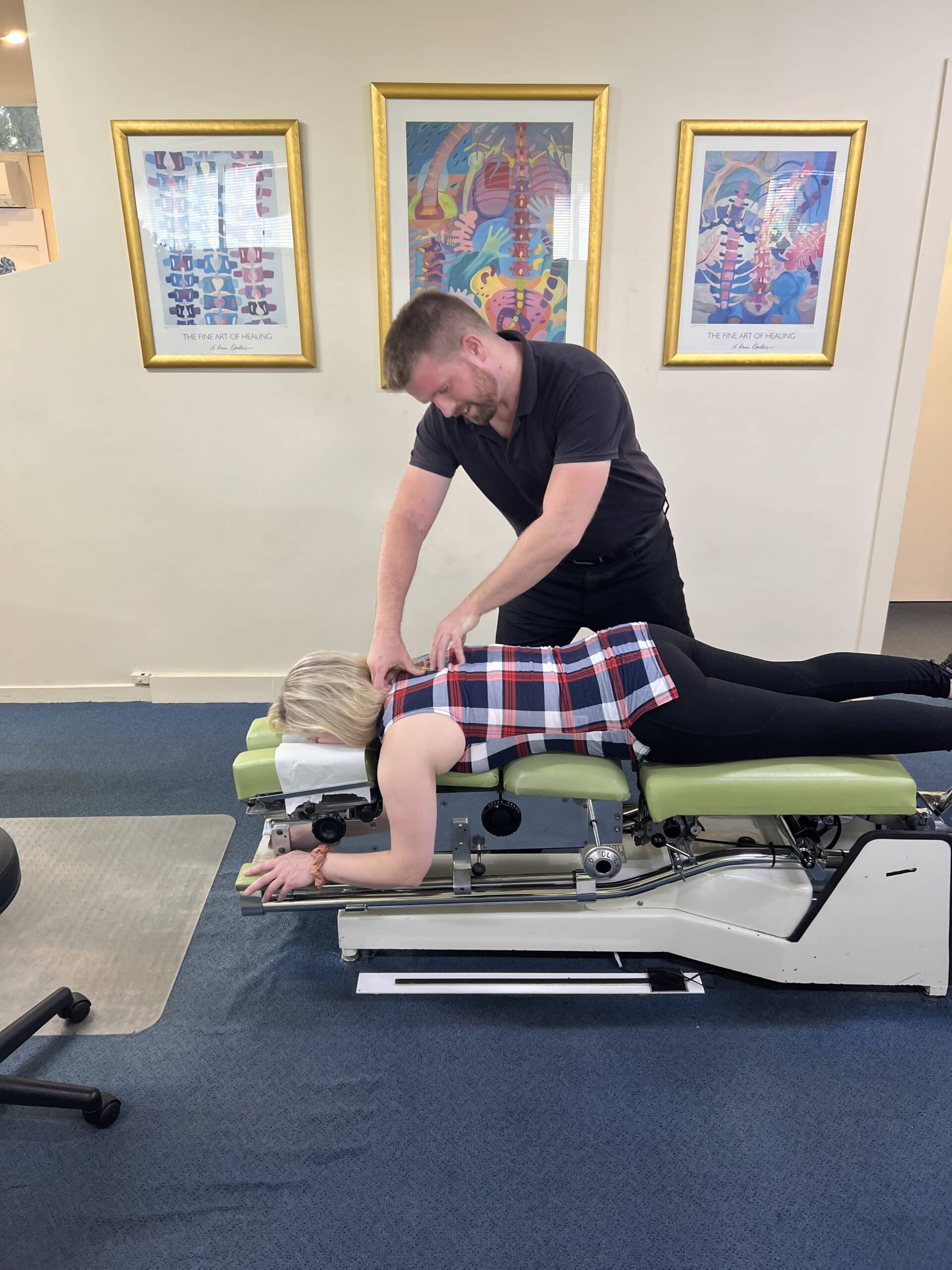
Care May Begin
Where clinically appropriate, care may begin on your first visit to help support relief.*
We offer both traditional hands-on chiropractic techniques and gentle, low-force approaches, tailored to your comfort. Care only proceeds with your consent.
Ready to Get Started?
Your first visit takes about 30 minutes. No referral needed, no lock-in plans. The decision is always yours.
Book Your First Visit*Subject to clinical assessment and suitability criteria. Bulk billing subject to eligibility criteria and clinical need.
How much does a chiropractor for cervicogenic headache cost in Adelaide?
Your first visit is over 40% below the South Australian average.
Source: Australian Chiropractors Association Consultation Fee Survey 2025 (SA data).
Care that fits your day
528 Marion Road, Plympton Park SA 5038
Ready to Get Started? We're Ready When You Are.
Choose a time that works for you. No referral needed.

Dr Sam Johnson (Chiropractor)
B.Sc.(Chiro), M.Chiro.(Macq)
$69
Initial Consultation
Up to 30 minutes, including full assessment
Book Your First VisitPrefer to call? (08) 8297 5277
Text: 0400 105 454 | Email: wecanhelp@stapletonchiropractic.com.au
You will receive a confirmation email with all details immediately after booking.
What causes neck pain?
Neck pain is most commonly caused by mechanical dysfunction in the joints, muscles, or discs of the cervical spine. Poor posture, prolonged desk work, smartphone use, stress, and acute injuries like whiplash are the leading triggers in working-age adults. Most neck pain may respond well to conservative care when the underlying cause is properly identified.
The cervical spine is made up of seven vertebrae, along with discs, joints, muscles, ligaments, and nerves that all work together to support your head and allow movement. When any of these structures are not functioning properly, pain and stiffness can develop.
Common contributing factors include:
- Cervical facet joint dysfunction (restricted or irritated joints in the neck)
- Muscle tension and strain (often from sustained postures or stress)
- Cervical disc issues (bulges, herniations, degeneration)
- Whiplash-associated disorders (from car accidents, falls, or impacts)
- Text neck and device-related strain (research suggests 64.6% of smartphone users report neck pain)[4]
- Poor workstation ergonomics and prolonged sitting
- Psychological stress and jaw clenching
- Sleep position and pillow issues
Who gets neck pain?
Neck pain affects people across all ages, though it peaks between 45 and 74 years. Women have a higher prevalence than men.[3] In Adelaide, we commonly see these groups:
Tap the one that sounds like you.
Office & Desk Workers
Screen time, forward head posture, ergonomics
Tradies & Physical Workers
Overhead work, vibration, heavy lifting
Nurses & Shift Workers
Patient handling, looking down, long shifts
Busy Parents
Breastfeeding posture, carrying, looking down
Drivers
Fixed posture, vibration, checking mirrors
Device & Screen Users
Text neck, gaming, scrolling posture
What conditions can present with neck pain?
Neck pain is often connected to other areas. Tap to learn more.
Headaches & Migraines
Tension, cervicogenic, recurring
Referred Pain
Shoulder, arm, or hand symptoms
Cervical Disc Issues
Bulges, herniations, degeneration
Whiplash
Post-accident neck injury
Thoracic Outlet Syndrome
Compression, tingling, numbness
Cervical Arthritis
Stiffness, degeneration, age-related
Jaw (TMJ) Dysfunction
Clenching, clicking, facial pain
When to seek urgent care for headaches
General information only (not a substitute for medical advice)
Most headaches, including cervicogenic headaches, are not caused by serious medical conditions, but some warning signs warrant prompt medical assessment. If any of the features below apply, contact your GP, call healthdirect on 1800 022 222, or call 000 for urgent symptoms.
Sudden, severe headache
A headache that comes on suddenly and reaches maximum intensity within seconds. This needs immediate medical assessment.
Headache with fever or neck stiffness
A headache combined with fever, neck stiffness, or a rash may indicate a serious infection and should be assessed urgently by a doctor.
Headache with neurological symptoms
A headache with vision changes, weakness, confusion, slurred speech, facial drooping, or unsteadiness needs immediate medical attention.
New headache pattern after age 50
A new or significantly different headache pattern after age 50, particularly with tenderness around the temples or jaw, should be assessed by a GP to exclude age-related conditions.
Headache after head or neck trauma
A headache following any head or neck injury, fall, or impact warrants prompt medical assessment, particularly if vomiting, drowsiness, or worsening symptoms occur.
Call 000 immediately if you experience a sudden severe headache, a headache with neurological symptoms (vision changes, weakness, confusion, slurred speech), or a headache after head or neck trauma.
Your first visit at Stapleton Chiropractic includes a detailed headache and neck history. If anything in your presentation suggests you should be assessed by a GP or medical services before starting chiropractic care, we’ll tell you and support referral.
💚 The health and wellbeing of you, your family, and your friends is our priority.
How does cervicogenic headache fit with other headache types?
Cervicogenic headache is one of several headache patterns that may present similarly. Research suggests 15 to 20% of chronic headaches may have a cervicogenic component, and mixed presentations (cervicogenic plus tension-type or migraine) are common. Understanding which pattern, or combination of patterns, applies to you is a core part of the assessment.
Cervicogenic headache is one of several primary headache patterns. Tension-type headache typically presents as a band-like pressure around the head, migraine as a throbbing one-sided pain often with nausea and light sensitivity, and cervicogenic headache as a referred pain from the upper neck. In clinical practice, mixed presentations are common, where features of two or more patterns overlap.
Research suggests that cervicogenic headache may be underdiagnosed because the pain is felt in the head rather than the neck. Patients often try treatments aimed at migraine or tension-type headache without a targeted assessment of the upper cervical spine. The distinction matters because the evidence base differs between headache types.
The 2026 Trager et al. clinical practice guideline recommends spinal manipulation as a primary intervention for cervicogenic headache. For tension-type headache, the same guideline recommends spinal manipulation within multimodal care. For migraine, evidence is developing but supportive of a possible role.
At Stapleton Chiropractic, the first step is a detailed headache history and a hands-on assessment to help work out which pattern, or combination of patterns, may be present. From there, we discuss your options in plain language.
Read the full overview of how we assess headaches and migraines →
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
How may chiropractic care help with cervicogenic headache?
The 2026 Trager et al. clinical practice guideline, published in the Journal of Integrative and Complementary Medicine, recommends spinal manipulation as a primary intervention for cervicogenic headache.[1] A 2020 systematic review and meta-analysis in the European Journal of Pain found that spinal manipulative therapy showed a significant effect on both pain intensity and headache frequency in patients with cervicogenic headache compared with control interventions.[2] Individual responses to care vary.
Care is hands-on and tailored to your presentation. Where joint restriction or muscle tension in the upper cervical spine is identified as a likely contributor, management may include spinal manipulation or mobilisation, targeted soft tissue work on the suboccipital muscles, and specific neck-mobility and deep neck-flexor exercises. Both traditional hands-on techniques and gentle, low-force approaches are available. We discuss your options before any care begins, and nothing proceeds without your consent.
Your initial assessment
Your initial assessment includes a detailed headache history (pattern, triggers, frequency, neck symptoms, medication use), red flag screening, and a hands-on examination of your cervical spine, suboccipital muscles, and upper thoracic region. The goal is to help explore whether mechanical factors may be contributing so we can discuss your options in plain language.
Tailored management approaches
Based on your assessment findings, management may include spinal manipulation or mobilisation targeted to the upper cervical spine, soft-tissue work on the suboccipital muscles, and a graduated program of neck-mobility and deep neck-flexor exercises. The 2018 Haas et al. dose-response randomised controlled trial suggests a dose-related effect between spinal manipulation and reduction in cervicogenic headache days.[3]
Gentle and low-force options available
Not everyone is comfortable with traditional manual adjustments, particularly around the upper neck. We offer a range of gentle, low-force techniques including instrument-assisted adjustments and sustained mobilisation. We discuss your options before any care begins, and nothing proceeds without your consent.
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
What does the research say about chiropractic for cervicogenic headache?
The 2026 Trager et al. clinical practice guideline, published in the Journal of Integrative and Complementary Medicine, recommends spinal manipulation as a primary intervention for cervicogenic headache.[1] A 2020 systematic review and meta-analysis in the European Journal of Pain found that spinal manipulative therapy showed a significant effect on both pain intensity and headache frequency in patients with cervicogenic headache compared with control interventions.[2] Individual responses to care vary.
The evidence base for chiropractic care in cervicogenic headache is among the strongest in the headache family, supported by a recent clinical practice guideline, systematic reviews, and dose-response randomised trials.
Trager et al. 2026 Clinical Practice Guideline
Updated chiropractic clinical practice guideline for headache disorders. Recommends spinal manipulation as a primary intervention for cervicogenic headache, and within multimodal care for tension-type headache. The strongest evidence-based endorsement of chiropractic for this specific headache type.[1]
Fernandez et al. 2020: Cervicogenic Headache
Systematic review and meta-analysis of spinal manipulation for cervicogenic headache. Found a significant effect on both pain intensity and headache frequency compared with control interventions. Heterogeneity across trials was moderate; evidence quality was rated as moderate.[2]
Haas et al. 2018: Dose-Response RCT
Dual-centre randomised controlled trial examining the dose-response relationship of spinal manipulation for cervicogenic headache. Found a dose-related effect on headache frequency, with higher treatment doses associated with greater reductions in headache days. Most frequently cited dose-response evidence for this condition.[3]
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
What the research says
“Spinal manipulative therapy showed a significant effect on pain intensity and frequency in patients with cervicogenic headache compared with control interventions.”
Fernandez et al., 2020 (European Journal of Pain)
“A dose-response relationship was observed between the number of spinal manipulation treatments and the reduction in cervicogenic headache days.”
Haas et al., 2018 (Spine Journal)
Why choose Stapleton Chiropractic for cervicogenic headaches?
Over 50 Years of Trusted Care
Stapleton Chiropractic has been part of the Plympton Park community since 1972. That is over 50 years of continuous operation supporting Adelaide families with their musculoskeletal health. We have seen how chiropractic care has evolved over five decades and we apply that experience to every patient we see.
Qualified, Registered, and Experienced
Dr Sam Johnson (Chiropractor) holds a Bachelor of Chiropractic Science and Master of Chiropractic from Macquarie University. He is registered with AHPRA and is a member of the Australian Chiropractors Association. Dr Johnson has been with the practice for over 10 years and became Principal Chiropractor in 2021.
Hours, Parking, and Pricing That Work
We are open 7am to 7pm weekdays and Saturday mornings, designed to fit around your work schedule. Free on-site parking. Your initial consultation is $69, well below the South Australian average of $122. All major private health funds accepted. No lock-in plans, no referral required.
Your Care, Your Choice
Whether you are looking for relief now or relief plus answers, your goals are our goals. We respect your autonomy at every step. No commitment to ongoing care, no lock-in plans. Where clinically appropriate, treatment may begin on your first visit.*
*Subject to clinical assessment and individual suitability.
Frequently asked questions about cervicogenic headache
Common questions from patients and from people searching online, answered by Dr Sam Johnson (Chiropractor).
Your initial consultation is $69, which is over 40% below the South Australian average of $122 (ACA Fee Survey 2025). Standard follow-up visits are $60. All major private health funds accepted, and we provide a receipt at the end of your visit so you can lodge your rebate via your fund’s app.
No lock-in plans. See our full pricing and health fund guide for details.
All major private health funds accepted. We provide a receipt at the end of your visit so you can claim your rebate via your fund’s app or member portal. The exact rebate amount depends on your level of cover.
Cervicogenic headache is typically one-sided, starts in the neck or base of the skull, is provoked by neck movement or sustained posture, and is often accompanied by restricted neck range of motion. Migraine is more commonly throbbing, may occur on either side, is often accompanied by nausea, light and sound sensitivity, and is usually not provoked by neck movement alone.
Mixed presentations are common, and a clinical assessment helps explore which pattern, or combination, may apply to you.
There is no single test for cervicogenic headache. Diagnosis is based on a detailed history and clinical examination, including headache features (one-sided, provoked by neck movement), findings on cervical range-of-motion testing, and reproduction of your headache with palpation of the upper cervical spine.
Imaging is not routinely required unless red flags are present. A chiropractor or GP with experience in headache assessment can help explore whether your pattern fits the cervicogenic profile.
Both. Spinal manipulation (the higher-velocity “click”) and mobilisation (slower, oscillatory movement) are both recognised techniques, and the choice depends on your presentation, preference, and comfort. The 2026 clinical practice guideline supports spinal manipulation as a primary intervention for cervicogenic headache.[1]
We explain both approaches before starting, and the decision is always yours.
Mixed presentations are common. Many people who experience cervicogenic headache also have occasional tension-type or migraine headaches, and vice versa. A careful assessment helps identify which pattern is most prominent and whether a cervicogenic component may be contributing.
For mixed cases, co-management with your GP is often helpful, and we are happy to correspond with your GP if that supports your care.
No. Chiropractors are primary contact practitioners, which means you can book directly without a GP referral. If we believe a GP assessment or referral to another practitioner would benefit you, we will let you know.
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
A calm, confident approach to your care


Continuing Stapleton Chiropractic’s 50-year legacy of trusted care in Adelaide’s south. We listen first, explain clearly, and focus on what matters most to you.
Where are you right now?
Choose the path that best describes where you are today.
Ready to Get Started? We're Ready When You Are.
Choose a time that works for you. No referral needed.

Dr Sam Johnson (Chiropractor)
B.Sc.(Chiro), M.Chiro.(Macq)
$69
Initial Consultation
Up to 30 minutes, including full assessment
Book Your First VisitPrefer to call? (08) 8297 5277
Text: 0400 105 454 | Email: wecanhelp@stapletonchiropractic.com.au
You will receive a confirmation email with all details immediately after booking.
What conditions may be related to cervicogenic headache?
Cervicogenic headache frequently coexists with other neck and shoulder conditions. Explore these related presentations.
Still researching? Read about what to expect at your first visit, our fees and health fund coverage, or explore our chiropractic services.
View References (5 citations)
References
- Trager RJ, Daniels CJ, Hawk C et al. (2026). Chiropractic management of adults with cervicogenic or tension-type headaches: development of a clinical practice guideline. Journal of Integrative and Complementary Medicine. PMID 41685545. DOI: 10.1177/27683605251397769. pubmed.ncbi.nlm.nih.gov
- Fernandez M et al. (2020). Spinal manipulation for the management of cervicogenic headache: a systematic review and meta-analysis. European Journal of Pain, 24(9):1687–1702. PMID 32621321. pubmed.ncbi.nlm.nih.gov
- Haas M, Bronfort G, Evans R et al. (2018). Dose-response and efficacy of spinal manipulation for care of cervicogenic headache: a dual-center randomized controlled trial. Spine Journal, 18(10):1741–1754. PMID 29481979. pubmed.ncbi.nlm.nih.gov
- Gross AR et al. (2015). Manipulation and mobilisation for neck disorders. Cochrane Database of Systematic Reviews. 51-trial Cochrane review including cervicogenic headache outcomes.
- National Institute for Health and Care Excellence. (2021). Headaches in over 12s: diagnosis and management. NICE Guideline CG150. nice.org.uk
Dr Sam Johnson (Chiropractor)
BSc(Chiro), MChiro, Macquarie University
Member, Australian Chiropractors Association
Stapleton Chiropractic | Est. 1972
528 Marion Road, Plympton Park SA 5038
(08) 8297 5277 | wecanhelp@stapletonchiropractic.com.au
Mon–Fri 7am–7pm | Sat 8am–12pm
Last clinically reviewed: April 2026 by Dr Sam Johnson (Chiropractor), B.Sc.(Chiro), M.Chiro.(Macq), AHPRA Registered.

