Sciatica Chiropractor in Adelaide


If sciatica is making it hard to sit through a meeting, sleep on your side, or get out of the car without wincing, you are not alone. I have spent over 10 years at Stapleton Chiropractic assessing patients who have been quietly pushing through radiating leg pain for weeks or months, often hoping it would settle on its own. Many have never had the lower back, pelvis, and nerve function properly examined together as one assessment.
My priority when you walk in is simple: help you feel better. From there, I take the time to explain what I am finding, what may be contributing, and what your options look like. Then the decision is yours. I will map out the path, but you are always in control.
I completed my Bachelor of Chiropractic Science and Master of Chiropractic at Macquarie University in Sydney. I work with people across all ages and walks of life, and I am as happy to co-manage your care with your GP as I am to refer on if something else suits you better.
If you have any questions, feel free to get in touch with our friendly team. I look forward to helping you with your sciatica.
Dr Sam Johnson (Chiropractor)
Principal Chiropractor, Stapleton Chiropractic
That burning pain shooting from your lower back into your leg, the pins and needles that wake you at night, the ache that flares every time you sit too long? The leg is where you feel it, but it usually starts somewhere else. Sciatica describes pain that travels along the sciatic nerve, most commonly from irritation at a nerve root in the lower back. At Stapleton Chiropractic, we start with a thorough hands-on assessment of your lower back, pelvis, and neurological function, explain what we find in plain language, and discuss your options.
Does this sound familiar?
Sciatica is pain that radiates along the sciatic nerve, typically from the lower back through the buttock and down one leg. At Stapleton Chiropractic in Adelaide (Est. 1972), a sciatica assessment costs $69 and includes focused neurological examination to help identify the likely contributing factors.
Yes, chiropractors in Adelaide commonly assess and manage sciatica and sciatic nerve pain. At Stapleton Chiropractic, we focus on identifying whether a nerve root in your lower back is being irritated, what is most likely to be driving the irritation, and whether conservative care is likely to help (or whether you need to be directed toward imaging, your GP, or a specialist opinion first). A detailed assessment is the starting point.
“Sciatica” is a symptom description rather than a single diagnosis. It refers to pain that travels along the path of the sciatic nerve, usually from the lower back, through the buttock, and down the back or side of the leg. Most episodes are triggered by a lumbar disc or nerve-root irritation, but other mechanisms include piriformis-related tension, spinal stenosis, and pregnancy-related changes. Research suggests the majority of sciatica episodes improve with conservative care over weeks to months. Individual responses vary.
What to Expect at Your First Visit
Your first visit is a 30-minute consultation costing $69. It includes a thorough hands-on assessment of your lower back, pelvis, and neurological function (reflexes, sensation, strength, straight-leg raise), a plain-language explanation of findings, and treatment on the same day where clinically appropriate. No referral is needed, and the decision about care is always yours.
Allow up to 30 minutes for a comprehensive initial consultation. Here is how it works.
You Tell Us
We listen carefully, ask the right questions, and build a clear picture of what has been going on with your neck.

We Assess
Hands-on testing and biostructural analysis to help explore whether a lumbar nerve root or local mechanical factor may be contributing to your leg pain.
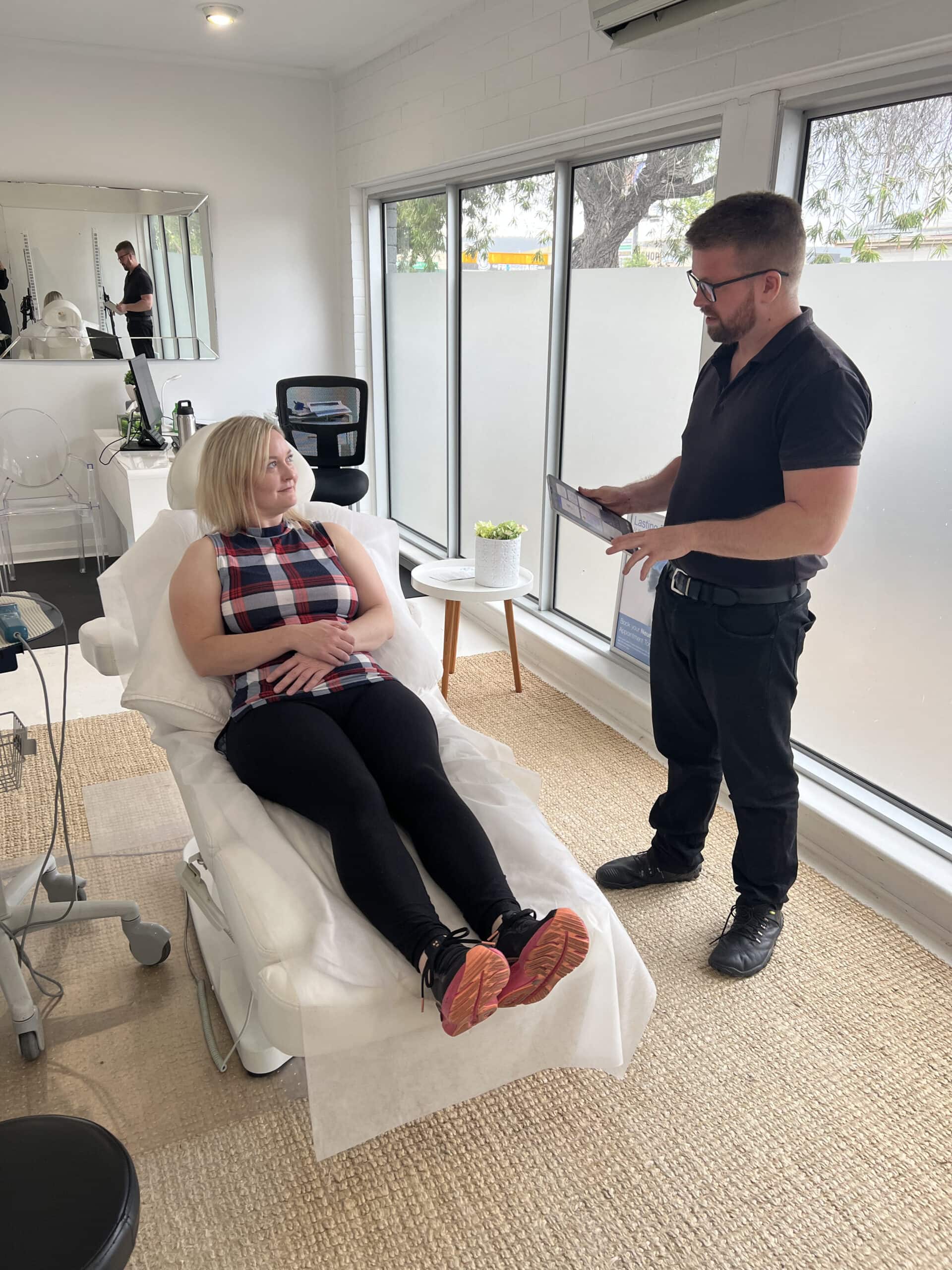
We Explain
We walk you through our findings and your options in plain language. If imaging is recommended, we will explain why and discuss your options.
X-rays are only taken with your agreement, and where eligible, may be bulk billed.*

Care May Begin
Where clinically appropriate, care may begin on your first visit to help support relief.*
We offer both traditional hands-on chiropractic techniques and gentle, low-force approaches, tailored to your comfort. Care only proceeds with your consent.
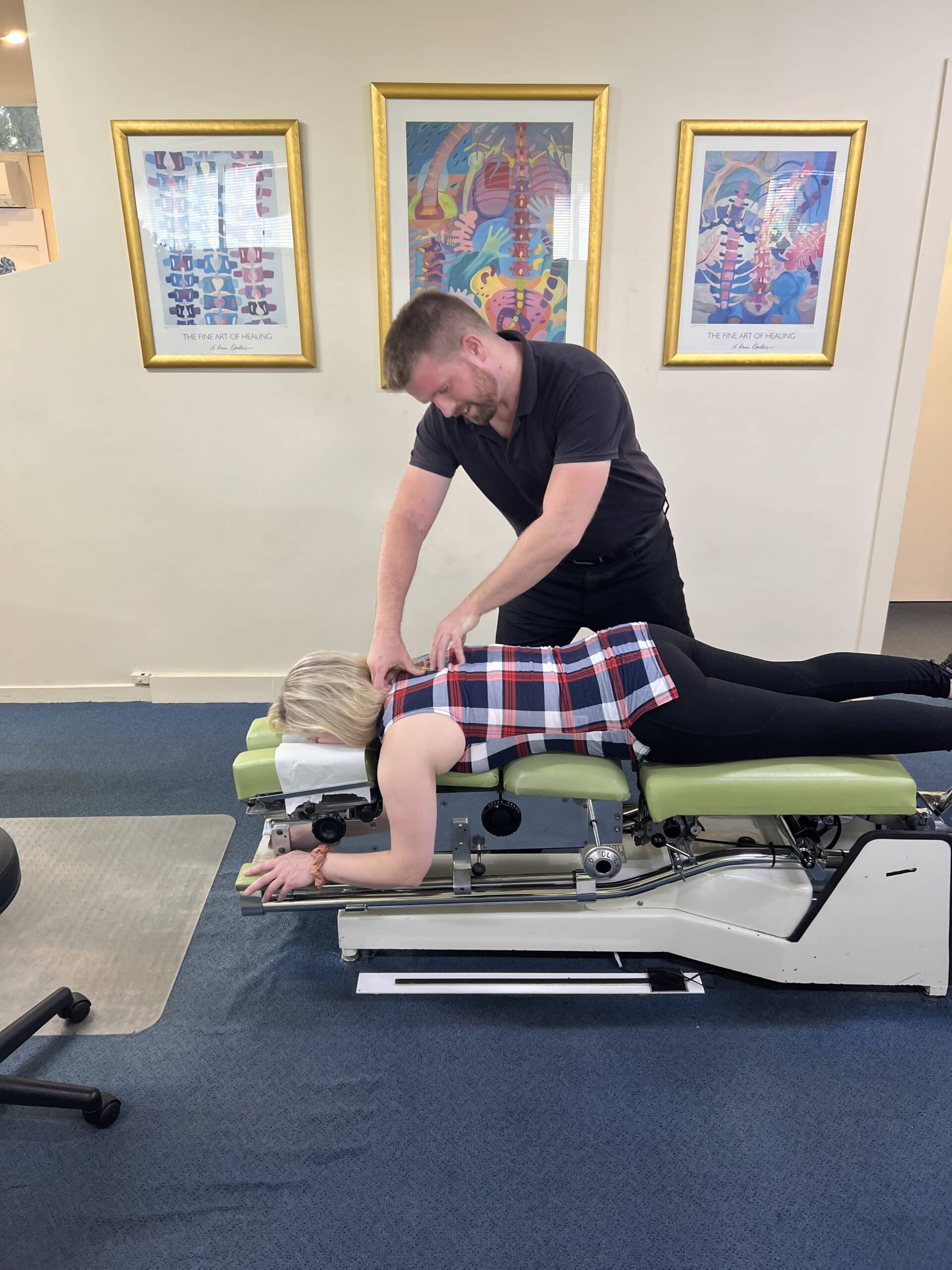
Ready to Get Started?
Your first visit takes about 30 minutes. No referral needed, no lock-in plans. The decision is always yours.
Book Your First Visit*Subject to clinical assessment and suitability criteria. Bulk billing subject to eligibility criteria and clinical need.
How much does a chiropractor for sciatica cost in Adelaide?
Your first visit is over 40% below the South Australian average.
Source: Australian Chiropractors Association Consultation Fee Survey 2025 (SA data).
What causes sciatica?
Sciatica is usually a symptom of something irritating a nerve root in the lower back or the sciatic nerve itself as it passes through the pelvis and hip. The most common contributor is a lumbar disc bulge or herniation, but piriformis tension, spinal stenosis, pregnancy-related changes, and sacroiliac joint dysfunction can all produce similar leg pain patterns. Identifying the likely mechanism is what guides the approach.
Common mechanical contributors we screen for at Stapleton Chiropractic:
- Lumbar disc bulge or herniation — the most common cause of sciatica. Disc material pressing on or irritating a lumbar nerve root (most often L4, L5, or S1) can refer pain, pins and needles, or numbness down the leg along a defined pattern. Research suggests disc herniation accounts for the majority of sciatica cases in adults under 50.
- Piriformis and gluteal tension — the sciatic nerve travels through the gluteal region near the piriformis muscle. Sustained tightness, trigger points, or compensatory tension in that area can irritate the nerve locally and produce buttock and leg symptoms without a lumbar nerve root being involved.
- Spinal stenosis — age-related narrowing of the spinal canal or the openings where nerve roots exit can compress the sciatic nerve roots, typically causing leg pain that is worse with standing or walking and eased by sitting or leaning forward. More common in adults over 50.
- Sacroiliac joint dysfunction — the sacroiliac joint, where the pelvis meets the lower spine, can refer pain into the buttock and thigh in a pattern that looks very much like sciatica. A thorough assessment helps separate SI joint-driven pain from a true lumbar nerve-root cause.
- Pregnancy and post-partum load changes — the combination of changing pelvic load, increased lumbar curvature, and ligamentous laxity during pregnancy can provoke sciatic-type pain, most often in the second and third trimesters. Symptoms may persist for a period after birth as the body adapts back.
- Prolonged sitting and sedentary load — long hours in a seated posture increase pressure within the lumbar discs, sustain load on the gluteal region, and can tighten the hip flexors. Research suggests sedentary work is associated with higher rates of sciatica and slower recovery from episodes.
Who gets sciatica?
Sciatica affects people across all ages and walks of life, with a lifetime incidence estimated between 13 and 40 percent across populations. In Adelaide, we commonly see these groups:
Tap the one that sounds like you.
Tradies & Manual Workers
Heavy lifting under flexion, twisting, repeated load
Truck & Delivery Drivers
Prolonged sitting, vibration, repeated in-and-out lifting
Office & Desk Workers
Prolonged sitting, static flexion, deconditioning
Nurses & Aged Care Workers
Patient handling, bending, twisting, night shift fatigue
Warehouse & Logistics Workers
Repeated lifting, bending, twisting, time pressure
Gym & Strength Athletes
Heavy deadlifting, squatting, spinal loading under fatigue
Economic impact: The lifetime incidence of sciatica is estimated between 13 and 40 percent, and low back pain (of which sciatica is a common variant) is the leading cause of disability globally (Global Burden of Disease Study).[10] Musculoskeletal injuries account for approximately 35.5% of all work-related injury and disease claims in Australia (Safe Work Australia).[12]
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
When to seek urgent care for sciatica
General information only — not a substitute for medical advice
Most sciatica is caused by mechanical irritation of a nerve root in the lower back and responds to conservative care over weeks to months. A small number of presentations involve warning signs that warrant prompt medical assessment. If any of the features below apply, contact your GP, call healthdirect on 1800 022 222, or call 000 for urgent symptoms.
New bladder or bowel changes
New difficulty passing or controlling urine, new bowel incontinence, or new numbness around the saddle region (inner thighs, groin, buttocks) warrants immediate emergency assessment. This combination of features in the context of sciatica can indicate a serious medical emergency. Go directly to a hospital emergency department.
Rapidly progressing leg weakness
Rapidly worsening weakness in one or both legs, a foot that is starting to drag or slap when you walk, or new difficulty lifting the foot or toes needs urgent medical assessment. Do not wait to see if it settles.
Saddle area numbness
New loss of sensation in the area that would contact a saddle (inner thighs, around the back passage, groin), particularly when combined with bladder or bowel symptoms, should be assessed immediately in an emergency department.
Severe pain with trauma
Severe lower back or leg pain following a fall, motor vehicle accident, or other significant trauma warrants prompt medical assessment before any manual therapy, to exclude fracture or serious injury.
Fever, weight loss, or night pain
Back or leg pain with fever, unexplained weight loss, night pain that wakes you from sleep, or a history of cancer should be assessed by a GP to help exclude infection or other age-related conditions before starting conservative care.
Call 000 or go to an emergency department immediately if you experience new bladder or bowel changes, saddle numbness, or rapidly progressing leg weakness alongside your sciatica. These are emergency features and must not be delayed.
Your first visit at Stapleton Chiropractic includes a detailed sciatica history and neurological screen. If anything in your presentation suggests you should be assessed by a GP or medical services before starting chiropractic care, we will tell you and support referral.
💚 The health and wellbeing of you, your family, and your friends is our priority.
Is your sciatica coming from a disc?
Often yes. Most sciatica is driven by irritation at a lumbar nerve root, and the most common reason that nerve root is irritated is a lumbar disc bulge or herniation. That said, not every case of sciatica is a disc, and the right starting point is a careful assessment, not a label.
The sciatic nerve is formed by the nerve roots that exit the lower back, mainly L4, L5, and S1. When one of those roots is irritated or compressed, pain, pins and needles, or numbness can travel along the path of the nerve into the buttock, thigh, calf, and foot. A lumbar disc bulge or herniation is the most frequent mechanism in people under 50; older adults more commonly have a mix of disc change and narrowing of the spinal canal.
The pattern of symptoms often gives useful clues. Pain that travels below the knee, is worse with coughing or sneezing, and follows a defined dermatome may be related to a lumbar nerve root. Pain that stays in the buttock and upper thigh and is reproduced by specific hip movements may be more related to the gluteal region than the spine. A proper assessment helps separate the two and guide treatment.
Management principles overlap whether the driver is a disc, local hip tension, or a combination, but the emphasis shifts. For a suspected disc with nerve-root involvement, clinical guidelines (including NICE NG59 and the American College of Physicians guideline) favour a graduated conservative approach with careful red-flag screening. For more locally driven presentations, hands-on care of the pelvis and gluteal region with rehabilitation may take priority.
If you want to understand the disc side of the picture in more detail, visit our slipped disc, herniated disc and sciatica page. It covers imaging, disc mechanisms, and conservative-versus-surgical considerations in depth. Read more about slipped disc, herniated disc and sciatica →
How may chiropractic care help with sciatica?
For mechanical lower back pain and lumbar radiculopathy (the clinical term for most sciatica), contemporary clinical guidelines including the UK NICE NG59 guideline and the US American College of Physicians guideline recommend non-pharmacological care as first-line management.[1][6] Spinal manipulation, mobilisation, and exercise are specifically listed as evidence-informed conservative options. Chiropractic care delivers these within a single provider, and where indicated we coordinate with GPs, imaging services, and specialist opinion.
Care is hands-on and tailored to your presentation. Depending on assessment findings and your preference, management may include lumbar mobilisation or manipulation, flexion-distraction or traction-style techniques for suspected disc-related presentations, targeted soft-tissue work through the gluteal and hip region, neural mobilisation, and a graduated exercise program. Low-force and gentler approaches are available if you are cautious, in acute pain, or pregnant. Nothing proceeds without your consent.
Your initial assessment
Your initial assessment includes a thorough history (mechanism of onset, pain pattern, what helps and hurts, red flag screen), a focused lumbar and hip examination, and a neurological screen (reflexes, sensation, strength, straight-leg raise, slump test where appropriate). We also look at how you move (walking, bending, sitting, and standing) because the movement signature often gives us more information than any single test.
Tailored management approaches
Based on your assessment findings, a management plan may combine spinal manipulation or mobilisation, flexion-distraction, soft-tissue work across the gluteal and hip region, neural mobilisation, and a graduated exercise program. The 2019 BMJ systematic review by Rubinstein et al. (47 RCTs, 9,211 participants) found spinal manipulative therapy produced similar effects to other recommended therapies for chronic low back pain, including patients with referred leg pain.[4]
Gentle and low-force options available
Not everyone is comfortable with traditional manual adjustments, particularly during an acute sciatic flare or in pregnancy. We offer a range of gentle, low-force techniques including instrument-assisted adjustments, mobilisation, flexion-distraction, and pregnancy-appropriate approaches. We discuss your options before any care begins, and nothing proceeds without your consent.
Comparing your options for sciatica
| Chiropractic | Physiotherapy | Cold Laser Therapy | |
|---|---|---|---|
| Primary focus | Lumbar and pelvic joint function, nerve-root mechanics, neurological screen, manual therapy and neural mobilisation where appropriate | Exercise rehabilitation, nerve mobility drills, movement retraining, graded return to activity | Soft-tissue inflammation and pain signalling at a cellular level via targeted light energy |
| Common techniques | Spinal manipulation, mobilisation, flexion-distraction, soft-tissue work, neural mobilisation, exercise prescription | Therapeutic exercise, motor-control retraining, dry needling, manual therapy, neural glides | Photobiomodulation applied to the lumbar paraspinals and gluteal region |
| Evidence base | NICE NG59 and ACP recommend SMT within multimodal care; Santilli 2006 RCT and McMorland 2010 RCT support benefit in carefully selected sciatica presentations | Strong evidence for exercise and graded activity across lower back pain and radiculopathy presentations | Lower-level evidence for lumbar and referred pain; often used alongside chiropractic care for pain and muscle tension |
| Referral needed? | No. Primary contact practitioner | No. Primary contact practitioner | No. Available here at Stapleton Chiropractic |
| Typical at Stapleton | History, red flag screen, lumbar and hip examination, neurological screen, manual therapy, neural mobilisation, exercise prescription | N/A — we can refer if physiotherapy is a better fit for your presentation | Multi-Radiance MR5 ACTIV PRO device, applied alongside chiropractic care where clinically appropriate |
| When to consider | Sciatica with or without a disc contributor, piriformis-related patterns, SI joint-driven leg pain, pregnancy-related sciatic pain | Presentations that are primarily exercise-rehab driven, or after an initial chiropractic assessment identifies that focus | Persistent buttock or leg soft-tissue pain, when a gentle non-manual approach is preferred |
Why this matters for you: Sciatica presentations vary widely. Some are acute and settle with a few weeks of graduated care, some are chronic and benefit from ongoing movement and load management, and a small number need imaging, specialist opinion, or surgical review. At Stapleton Chiropractic we offer both chiropractic care and cold laser therapy under the one roof, so Dr Sam can assess your presentation and discuss which approach, or combination, may be most appropriate for you.
If your presentation suggests a different type of care would suit you better, we will let you know and can refer to an appropriate practitioner. Interested in whether cold laser may be appropriate for your sciatica? Simply mention it during your initial consultation with Dr Sam.
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
What does the research say about chiropractic for sciatica?
Contemporary clinical practice guidelines (the UK NICE NG59 guideline and the US American College of Physicians 2017 guideline) recommend non-pharmacological care as first-line management for low back pain with or without sciatica.[1][6] Spinal manipulation, mobilisation, and exercise are specifically listed as evidence-informed conservative options. Chiropractic care delivers these within a single provider, and where indicated we coordinate with GPs, imaging services, and specialist opinion.
Evidence for manual therapy in sciatica and lumbar radiculopathy is supportive in carefully selected cases. Published trials include comparisons with simulated manipulation and with surgical microdiscectomy.
NICE NG59: Low Back Pain and Sciatica Guideline
UK National Institute for Health and Care Excellence guideline on non-invasive management of low back pain and sciatica in people over 16. Recommends considering manual therapy (including spinal manipulation and mobilisation) as part of a treatment package alongside exercise. Cautions against routine imaging for non-specific presentations and highlights conservative management before surgical referral.[1]
Santilli et al. 2006: 102-Patient Double-Blind RCT
Randomised double-blind clinical trial of 102 patients with acute back pain and sciatica with disc protrusion, comparing active spinal manipulation with simulated manipulation. Active manipulation was associated with significantly greater relief of both local and radiating pain at six months compared with the simulated group, with no adverse events reported.[2]
McMorland et al. 2010: Manipulation vs Microdiscectomy
Prospective randomised clinical study of patients with sciatica secondary to lumbar disc herniation who had failed at least three months of non-operative management. Approximately 60% of patients who received spinal manipulation reported benefits comparable to those who had surgical microdiscectomy at one-year follow-up. Patients who did not respond to manipulation achieved good outcomes with subsequent surgery.[3]
Rubinstein et al. 2019: BMJ Meta-Analysis (Chronic LBP)
Systematic review and meta-analysis of 47 RCTs (9,211 participants) on spinal manipulative therapy for chronic low back pain, including patients with referred leg pain. Found that SMT produced similar effects to other recommended therapies for pain and small improvements in function. Adverse events were generally minor and transient.[4]
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
What the research says
“Consider manual therapy (spinal manipulation, mobilisation or soft-tissue techniques such as massage) for managing low back pain with or without sciatica, but only as part of a treatment package including exercise, with or without psychological therapy.”
NICE Guideline NG59, 2016 (updated 2020)
“Clinicians and patients should initially select non-pharmacologic treatment [for low back pain], including spinal manipulation.”
American College of Physicians Clinical Practice Guideline, Qaseem et al., 2017
Why choose Stapleton Chiropractic for sciatica?
Over 50 Years of Trusted Care
Stapleton Chiropractic has been part of the Plympton Park community since 1972. That is over 50 years of continuous operation supporting Adelaide families with their musculoskeletal health. We have seen how chiropractic care has evolved over five decades and we apply that experience to every patient we see.
Qualified, Registered, and Experienced
Dr Sam Johnson (Chiropractor) holds a Bachelor of Chiropractic Science and Master of Chiropractic from Macquarie University. He is registered with AHPRA and is a member of the Australian Chiropractors Association. Dr Johnson has been with the practice for over 10 years and became Principal Chiropractor in 2021.
Hours, Parking, and Pricing That Work
We are open 7am to 7pm weekdays and Saturday mornings, designed to fit around your work schedule. Free on-site parking. Your initial consultation is $69, well below the South Australian average of $122. All major private health funds accepted. No lock-in plans, no referral required.
Your Care, Your Choice
Whether you are looking for relief now or relief plus answers, your goals are our goals. We respect your autonomy at every step. No commitment to ongoing care, no lock-in plans. Where clinically appropriate, treatment may begin on your first visit.*
*Subject to clinical assessment and individual suitability.
Frequently asked questions about sciatica
Common questions from patients and from people searching online, answered by Dr Sam Johnson (Chiropractor).
Your initial consultation is $69, which is over 40% below the South Australian average of $122 (ACA Fee Survey 2025). Standard follow-up visits are $60. All major private health funds accepted, and we provide a receipt at the end of your visit so you can lodge your rebate via your fund’s app.
No lock-in plans, no pressure. See our full pricing and health fund guide for details.
Allow up to 30 minutes. We take a detailed history (mechanism of onset, pain pattern, what makes it better or worse, a red flag screen) and perform a focused lumbar and neurological examination. We explain our findings in plain language, outline options including when a GP review or imaging may be warranted, and where clinically appropriate, care may begin on your first visit. The decision about care is always yours.
Learn more about what to expect at your first visit.
You do not need a GP referral to see a chiropractor in Australia, so either starting point is reasonable. If your sciatica came on suddenly with any of the red flags listed above (bladder or bowel changes, saddle numbness, rapidly progressing weakness), start with your GP or an emergency department. If it is a more typical mechanical presentation, starting with a chiropractic assessment is a common path, and we will happily coordinate with your GP if imaging or further review is indicated.
“Fix” is a word we avoid because outcomes depend on many individual factors. What chiropractic care may offer is a structured approach to managing sciatica, including manual therapy, mobilisation, soft-tissue work, and rehabilitation exercises. Research suggests conservative care is a reasonable first-line approach for most presentations, but individual responses vary and some presentations need medical or specialist input.
Many people with sciatica are managed conservatively and may benefit from hands-on care, but it is not a one-size-fits-all situation. A careful assessment helps identify whether the presentation is appropriate for manual therapy, which techniques are suitable, and whether a gentler or lower-force approach may be more appropriate in your case. Where red flags are present, we direct you to medical services first.
Research suggests many episodes of sciatica improve over weeks to months, particularly when movement is maintained and aggravating factors are addressed (NICE NG59).[1] That said, “wait and see” is not always the best option, especially if pain is severe or function is affected. A conservative care plan may help shorten recovery and reduce recurrence, and can often be paused or stepped down once you are making good progress.
Not always. Clinical guidelines (including NICE NG59) caution against routine imaging for non-specific low back pain and sciatica because imaging often shows changes that are not the cause of symptoms. Imaging is indicated when red flags are present, when progress is not being made as expected, or when a specialist opinion is being considered. We are happy to coordinate with your GP on imaging if it is appropriate.
Sciatica describes the symptom (pain along the path of the sciatic nerve), while “slipped disc” is a common description for a disc bulge, herniation, or prolapse in the lower back. A slipped disc is the most common cause of sciatica, but not the only one. You can also have a slipped disc without sciatica if the disc is not irritating a nerve root. Our slipped disc, herniated disc and sciatica page covers the disc side of the picture in more detail.
Pregnancy-related sciatic pain is common, particularly in the second and third trimesters, and many pregnant patients see chiropractors for it. We use lower-force, pregnancy-appropriate techniques where clinically indicated. As with any condition, we screen carefully before care begins and coordinate with your GP or obstetric team if anything in your presentation warrants it.
All major private health funds accepted. We provide a receipt at the end of your visit so you can claim your rebate via your fund’s app or member portal. The exact rebate amount depends on your level of cover.
No. Chiropractors are primary contact practitioners, which means you can book directly without a GP referral. If we believe a referral to your GP or another practitioner would benefit you, we will let you know and support that process.
Our goal is to help you become as independent as possible. How often you visit, and for how long, is always your decision. We provide recommendations based on your progress and aim to reduce frequency as you improve, but there are no lock-in plans.
*All care is provided subject to clinical assessment and individual suitability. Individual responses to treatment vary.
A calm, confident approach to your care


Continuing Stapleton Chiropractic’s 50-year legacy of trusted care in Adelaide’s south. We listen first, explain clearly, and focus on what matters most to you.
Where are you right now?
Choose the path that best describes where you are today.
Ready to Get Started? We're Ready When You Are.
Choose a time that works for you. No referral needed.

Dr Sam Johnson (Chiropractor)
B.Sc.(Chiro), M.Chiro.(Macq)
$69
Initial Consultation
Up to 30 minutes, including full assessment
Book Your First VisitPrefer to call? (08) 8297 5277
Text: 0400 105 454 | Email: wecanhelp@stapletonchiropractic.com.au
You will receive a confirmation email with all details immediately after booking.
What conditions may be related to sciatica?
Sciatica often overlaps with other spinal and lower-limb presentations. Explore these related concerns.
Still researching? Read about what to expect at your first visit, our fees and health fund coverage, or explore our chiropractic services.
View References (12 citations)
References
- National Institute for Health and Care Excellence. (2016, updated 2020). Low back pain and sciatica in over 16s: assessment and management. NICE Guideline NG59. nice.org.uk
- Santilli V, Beghi E, Finucci S. (2006). Chiropractic manipulation in the treatment of acute back pain and sciatica with disc protrusion: a randomized double-blind clinical trial of active and simulated spinal manipulations. The Spine Journal, 6(2):131–137. PMID 16517383. pubmed.ncbi.nlm.nih.gov
- McMorland G, Suter E, Casha S, du Plessis SJ, Hurlbert RJ. (2010). Manipulation or microdiskectomy for sciatica? A prospective randomized clinical study. Journal of Manipulative and Physiological Therapeutics, 33(8):576–584. PMID 21036279. pubmed.ncbi.nlm.nih.gov
- Rubinstein SM, de Zoete A, van Middelkoop M, Assendelft WJJ, de Boer MR, van Tulder MW. (2019). Benefits and harms of spinal manipulative therapy for the treatment of chronic low back pain: systematic review and meta-analysis of randomised controlled trials. BMJ, 364:l689. PMID 30867144. pubmed.ncbi.nlm.nih.gov
- Paige NM, Miake-Lye IM, Booth MS et al. (2017). Association of spinal manipulative therapy with clinical benefit and harm for acute low back pain: systematic review and meta-analysis. JAMA, 317(14):1451–1460. PMID 28399251. pubmed.ncbi.nlm.nih.gov
- Qaseem A, Wilt TJ, McLean RM, Forciea MA. (2017). Noninvasive treatments for acute, subacute, and chronic low back pain: a clinical practice guideline from the American College of Physicians. Annals of Internal Medicine, 166(7):514–530. PMID 28192789. pubmed.ncbi.nlm.nih.gov
- Bronfort G, Haas M, Evans R, Leininger B, Triano J. (2010). Effectiveness of manual therapies: the UK evidence report. Chiropractic & Osteopathy, 18:3. PMID 20184717. pubmed.ncbi.nlm.nih.gov
- Foster NE, Anema JR, Cherkin D et al. (2018). Prevention and treatment of low back pain: evidence, challenges, and promising directions. The Lancet, 391(10137):2368–2383. PMID 29573872. pubmed.ncbi.nlm.nih.gov
- Konstantinou K, Dunn KM. (2008). Sciatica: review of epidemiological studies and prevalence estimates. Spine, 33(22):2464–2472. [PMID verification pending]
- Global Burden of Disease Study Collaborators. (2020). Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019. The Lancet, 396(10258):1204–1222.
- Australian Institute of Health and Welfare. (2023). Back problems: overview. aihw.gov.au
- Safe Work Australia. Musculoskeletal injury statistics. safeworkaustralia.gov.au
Dr Sam Johnson (Chiropractor)
BSc(Chiro), MChiro, Macquarie University
Member, Australian Chiropractors Association
Stapleton Chiropractic | Est. 1972
528 Marion Road, Plympton Park SA 5038
(08) 8297 5277 | wecanhelp@stapletonchiropractic.com.au
Mon–Fri 7am–7pm | Sat 8am–12pm
Last clinically reviewed: April 2026 by Dr Sam Johnson (Chiropractor), B.Sc.(Chiro), M.Chiro.(Macq), AHPRA Registered.
Last clinically reviewed: 19 April 2026 by Dr Sam Johnson (Chiropractor)

